Blog
Bunion Complications
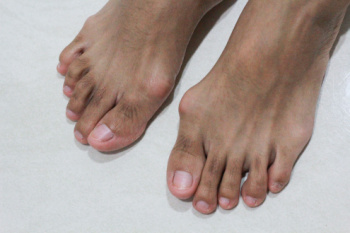
A bunion is a bony bump that forms on the joint at the base of the big toe, often causing the toe to deviate towards the others. Common issues can include chronic pain, bursitis or inflammation of the fluid-filled pads that cushion the bones, and metatarsalgia or pain and inflammation in the ball of the foot. Severe cases or complications can lead to hammertoes or crossover toes, where toes bend abnormally, and even arthritis in the big toe joint. Preventing bunion complications involves wearing properly fitted shoes with a wide toe box, avoiding high heels, and using orthotic inserts to reduce pressure on the bunion. Maintaining a healthy weight can also alleviate stress on the feet. Treatment options range from non-surgical methods like padding and medications to manage pain to surgical procedures for more severe cases. If you have a bunion that is causing worsening symptoms, it is suggested that you promptly consult a podiatrist who can help to manage symptoms and prevent further complications.
If you are suffering from bunion pain, contact one of our podiatrists of James Kutchback, DPM, CWS-P. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
- Genetics – some people inherit feet that are more prone to bunion development
- Inflammatory Conditions - rheumatoid arthritis and polio may cause bunion development
Symptoms
- Redness and inflammation
- Pain and tenderness
- Callus or corns on the bump
- Restricted motion in the big toe
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact our offices located in The Woodlands and Woodville, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Diabetic Neuropathy

Diabetic neuropathy is a serious complication of diabetes that results from nerve damage caused by prolonged high blood sugar and elevated blood fats. This condition often targets the nerves in the lower legs and feet, leading to what is known as peripheral neuropathy. Studies show that between one-third and one-half of people with diabetes will experience this condition. Diabetic neuropathy can bring on a range of uncomfortable symptoms, including numbness and weakness, burning, tingling, and pain in the lower limbs. Additionally, the diminished sensation can make you more susceptible to unnoticed wounds on your feet, which increases the risk of infections and complications. To manage diabetic neuropathy effectively, it is suggested you schedule an appointment with a podiatrist, ensuring that any potential issues are caught early and treated appropriately.
Neuropathy
Neuropathy can be a potentially serious condition, especially if it is left undiagnosed. If you have any concerns that you may be experiencing nerve loss in your feet, consult with one of our podiatrists from James Kutchback, DPM, CWS-P. Our doctors will assess your condition and provide you with quality foot and ankle treatment for neuropathy.
What Is Neuropathy?
Neuropathy is a condition that leads to damage to the nerves in the body. Peripheral neuropathy, or neuropathy that affects your peripheral nervous system, usually occurs in the feet. Neuropathy can be triggered by a number of different causes. Such causes include diabetes, infections, cancers, disorders, and toxic substances.
Symptoms of Neuropathy Include:
- Numbness
- Sensation loss
- Prickling and tingling sensations
- Throbbing, freezing, burning pains
- Muscle weakness
Those with diabetes are at serious risk due to being unable to feel an ulcer on their feet. Diabetics usually also suffer from poor blood circulation. This can lead to the wound not healing, infections occurring, and the limb may have to be amputated.
Treatment
To treat neuropathy in the foot, podiatrists will first diagnose the cause of the neuropathy. Figuring out the underlying cause of the neuropathy will allow the podiatrist to prescribe the best treatment, whether it be caused by diabetes, toxic substance exposure, infection, etc. If the nerve has not died, then it’s possible that sensation may be able to return to the foot.
Pain medication may be issued for pain. Electrical nerve stimulation can be used to stimulate nerves. If the neuropathy is caused from pressure on the nerves, then surgery may be necessary.
If you have any questions, please feel free to contact our offices located in The Woodlands and Woodville, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Preventing Blisters While Playing Tennis
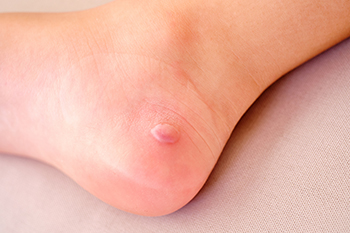
Playing tennis can be tough on the feet due to the high-impact movements and frequent lateral actions that can often lead to painful blisters. These blisters result from the friction between the skin and footwear, which is inevitable during extended matches. While preventive measures like wearing moisture-wicking socks and properly fitted shoes can reduce the risk, sometimes blisters still develop. When this happens, it may help to consult a podiatrist. This foot doctor can provide professional treatment to alleviate pain and promote healing, ensuring you will not have to pause your tennis activities for long. Specialized padding techniques, specific footwear adjustments, or custom orthotics may be offered to minimize future friction. A podiatrist also can provide personalized advice tailored to your specific foot structure and playing style, which can help prevent blisters from recurring. If you frequently develop blisters on the feet, it is suggested that you schedule an appointment with a podiatrist for effective treatment and prevention methods.
Blisters are prone to making everyday activities extremely uncomfortable. If your feet are hurting, contact one of our podiatrists of James Kutchback, DPM, CWS-P. Our doctors can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters develop as a result of constantly wearing tight or ill-fitting footwear. This happens due to the constant rubbing from the shoe, which can often lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
How Do Blisters Form?
Blisters on the feet are often the result of constant friction of skin and material, usually by shoe rubbing. Walking in sandals, boots, or shoes that don’t fit properly for long periods of time can result in a blister. Having consistent foot moisture and humidity can easily lead to blister formation.
Prevention & Treatment
It is important to properly care for the affected area in order to prevent infection and ease the pain. Do not lance the blister and use a Band-Aid to provide pain relief. Also, be sure to keep your feet dry and wear proper fitting shoes. If you see blood or pus in a blister, seek assistance from a podiatrist.
If you have any questions, please feel free to contact our offices located in The Woodlands and Woodville, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Custom Orthotics for Kids With Flexible Flat Feet
 Flexible flat feet in children, also known as pediatric flatfoot, is a condition where the arch of the foot collapses upon standing but reappears when sitting or on tiptoes. This common condition often resolves with age, but in some cases, intervention is necessary. Custom orthotics are specially designed shoe inserts tailored to an individual's foot structure. For children with flexible flat feet, these orthotics provide support to the arch, enhance foot alignment, and reduce strain on muscles and ligaments. They can alleviate pain and prevent potential future issues related to improper foot mechanics. The duration for wearing custom orthotics varies, often spanning several months to years, depending on the severity of the condition and the child's growth. Continuous monitoring and adjustments ensure optimal benefits. For personalized advice and to determine if custom orthotics are appropriate for your child, it is suggested that you consult a podiatrist.
Flexible flat feet in children, also known as pediatric flatfoot, is a condition where the arch of the foot collapses upon standing but reappears when sitting or on tiptoes. This common condition often resolves with age, but in some cases, intervention is necessary. Custom orthotics are specially designed shoe inserts tailored to an individual's foot structure. For children with flexible flat feet, these orthotics provide support to the arch, enhance foot alignment, and reduce strain on muscles and ligaments. They can alleviate pain and prevent potential future issues related to improper foot mechanics. The duration for wearing custom orthotics varies, often spanning several months to years, depending on the severity of the condition and the child's growth. Continuous monitoring and adjustments ensure optimal benefits. For personalized advice and to determine if custom orthotics are appropriate for your child, it is suggested that you consult a podiatrist.
If you are having discomfort in your feet and would like to try orthotics, contact one of our podiatrists from James Kutchback, DPM, CWS-P. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Are Orthotics?
Orthotics are inserts you can place into your shoes to help with a variety of foot problems such as flat feet or foot pain. Orthotics provide relief and comfort for minor foot and heel pain but can’t correct serious biomechanical problems in your feet.
Over-the-Counter Inserts
Orthotics come in a wide variety of over-the-counter inserts that are used to treat foot pain, heel pain, and minor problems. For example, arch supports can be inserted into your shoes to help correct overarched or flat feet, while gel insoles are often used because they provide comfort and relief from foot and heel pain by alleviating pressure.
Prescription Orthotics
If over-the-counter inserts don’t work for you or if you have a more severe foot concern, it is possible to have your podiatrist prescribe custom orthotics. These high-quality inserts are designed to treat problems such as abnormal motion, plantar fasciitis, and severe forms of heel pain. They can even be used to help patients suffering from diabetes by treating foot ulcers and painful calluses and are usually molded to your feet individually, which allows them to provide full support and comfort.
If you are experiencing minor to severe foot or heel pain, it’s recommended to speak with your podiatrist about the possibilities of using orthotics. A podiatrist can determine which type of orthotic is right for you and allow you to take the first steps towards being pain-free.
If you have any questions, please feel free to contact our offices located in The Woodlands and Woodville, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Possible Causes of Foot Pain
 Foot pain is a common issue that can arise from various causes, impacting daily activities and overall quality of life. The most common causes include plantar fasciitis, which involves inflammation of the tissue running along the bottom of the foot, and arthritis, which affects the joints. Other frequent sources of foot pain are bunions, caused by misalignment of the big toe joint, and hammertoes, where toes bend abnormally. Injuries such as fractures, sprains, and strains also contribute to foot pain, often resulting from accidents or overuse. Additionally, deformities like flat feet or high arches can lead to discomfort by altering the natural distribution of weight across the foot. Conditions such as tendinitis and neuropathy, particularly in individuals with diabetes, can further contribute to foot pain. Treatment varies depending on the cause but typically includes rest, anti-inflammatory medications, and wearing proper footwear. Stretching exercises and orthotic devices can also help alleviate pain. For persistent or severe foot pain, it is suggested that you consult a podiatrist for a comprehensive diagnosis and tailored treatment plan.
Foot pain is a common issue that can arise from various causes, impacting daily activities and overall quality of life. The most common causes include plantar fasciitis, which involves inflammation of the tissue running along the bottom of the foot, and arthritis, which affects the joints. Other frequent sources of foot pain are bunions, caused by misalignment of the big toe joint, and hammertoes, where toes bend abnormally. Injuries such as fractures, sprains, and strains also contribute to foot pain, often resulting from accidents or overuse. Additionally, deformities like flat feet or high arches can lead to discomfort by altering the natural distribution of weight across the foot. Conditions such as tendinitis and neuropathy, particularly in individuals with diabetes, can further contribute to foot pain. Treatment varies depending on the cause but typically includes rest, anti-inflammatory medications, and wearing proper footwear. Stretching exercises and orthotic devices can also help alleviate pain. For persistent or severe foot pain, it is suggested that you consult a podiatrist for a comprehensive diagnosis and tailored treatment plan.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with one of our podiatrists from James Kutchback, DPM, CWS-P. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact our offices located in The Woodlands and Woodville, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Symptoms of a Sprained Ankle
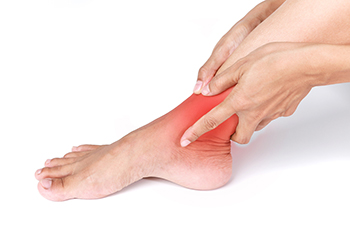 A sprained ankle occurs when the ligaments that support the ankle stretch or tear due to sudden twisting, rolling, or turning of the foot. This injury is common in sports, walking on uneven surfaces, or missteps that put the ankle in an awkward position. Symptoms of a sprained ankle can include pain, swelling, bruising, and difficulty bearing weight on the affected foot. You might also hear a popping sound at the time of the injury. To determine if you have a sprain, pay attention to the severity of pain and swelling, any instability in the ankle, and whether the pain worsens with movement. Initial treatment for a sprained ankle involves rest, compression, and elevation. Avoid putting weight on the ankle and consider using crutches. Anti-inflammatory pain relievers can help manage pain and discomfort. Proper rehabilitation, including targeted stretching exercises, is essential for healing and preventing future injuries. If you think you have sprained your ankle, it is suggested that you schedule an appointment with a podiatrist for an accurate diagnosis and comprehensive treatment plan.
A sprained ankle occurs when the ligaments that support the ankle stretch or tear due to sudden twisting, rolling, or turning of the foot. This injury is common in sports, walking on uneven surfaces, or missteps that put the ankle in an awkward position. Symptoms of a sprained ankle can include pain, swelling, bruising, and difficulty bearing weight on the affected foot. You might also hear a popping sound at the time of the injury. To determine if you have a sprain, pay attention to the severity of pain and swelling, any instability in the ankle, and whether the pain worsens with movement. Initial treatment for a sprained ankle involves rest, compression, and elevation. Avoid putting weight on the ankle and consider using crutches. Anti-inflammatory pain relievers can help manage pain and discomfort. Proper rehabilitation, including targeted stretching exercises, is essential for healing and preventing future injuries. If you think you have sprained your ankle, it is suggested that you schedule an appointment with a podiatrist for an accurate diagnosis and comprehensive treatment plan.
Ankle and foot injuries are common among athletes and in many sports. They can be caused by several problems and may be potentially serious. If you are feeling pain or think you were injured in a sporting event or when exercising, consult with one of our podiatrists from James Kutchback, DPM, CWS-P. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Common Injuries
The most common injuries that occur in sporting activities include:
- Achilles Tendonitis
- Achilles Tendon Rupture
- Ankle Sprains
- Broken Foot
- Plantar Fasciitis
- Stress Fractures
- Turf Toe
Symptoms
Symptoms vary depending upon the injury and in some cases, there may be no symptoms at all. However, in most cases, some form of symptom is experienced. Pain, aching, burning, bruising, tenderness, tightness or stiffness, sensation loss, difficulty moving, and swelling are the most common symptoms.
Treatment
Just as symptoms vary depending upon the injury, so do treatment options. A common treatment method is known as the RICE method. This method involves rest, applying ice, compression and elevating the afflicted foot or ankle. If the injury appears to be more serious, surgery might be required, such as arthroscopic or reconstructive surgery. Lastly, rehabilitation or therapy might be needed to gain full functionality in the afflicted area. Any discomfort experienced by an athlete must be evaluated by a licensed, reputable medical professional.
If you have any questions please contact our offices located in The Woodlands and Woodville, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
The Hidden Dangers of Flip-Flops on Your Feet
 Flip-flops, though convenient, can be harsh on your feet, especially for individuals at risk like those with diabetes. The lack of support in flip-flops leads to improper heel strike, causing stress on the heels and increasing the risk of plantar fasciitis. Further, to keep the flip flops on, wearers often grip with their toes, which can cause muscle strain and negatively affect conditions like hammertoes. For people with diabetes, the minimal protection provided by flip-flops increases the risk of cuts, blisters, and infections due to decreased sensation and poor wound healing. Additionally, the flat design offers little or no arch support, leading to pain and discomfort in the feet and ankles. If you have foot pain as a result of wearing flip-flops, it is suggested that you consult a podiatrist who can offer you relief tips, in addition to guiding you on more favorable footwear choices.
Flip-flops, though convenient, can be harsh on your feet, especially for individuals at risk like those with diabetes. The lack of support in flip-flops leads to improper heel strike, causing stress on the heels and increasing the risk of plantar fasciitis. Further, to keep the flip flops on, wearers often grip with their toes, which can cause muscle strain and negatively affect conditions like hammertoes. For people with diabetes, the minimal protection provided by flip-flops increases the risk of cuts, blisters, and infections due to decreased sensation and poor wound healing. Additionally, the flat design offers little or no arch support, leading to pain and discomfort in the feet and ankles. If you have foot pain as a result of wearing flip-flops, it is suggested that you consult a podiatrist who can offer you relief tips, in addition to guiding you on more favorable footwear choices.
Flip-flops can cause a lot of problems for your feet. If you have any concerns about your feet or ankles, contact one of our podiatrists from James Kutchback, DPM, CWS-P. Our doctors will assist you with all of your foot and ankle needs.
Flip-Flops and Feet
Flip-flops have managed to become a summer essential for a lot of people. While the shoes may be stylish and easy to slip on and off, they can be dangerous to those who wear them too often. These shoes might protect you from fungal infections such as athlete’s foot, but they can also give you foot pain and sprained ankles if you trip while wearing them.
When Are They Okay to Wear?
Flip-flops should only be worn for very short periods of time. They can help protect your feet in places that are crawling with fungi, such as gym locker rooms. Athlete’s foot and plantar warts are two common fungi that flip-flops may help protect your feet against.
Why Are They Bad for My Feet?
These shoes do not offer any arch support, so they are not ideal for everyday use. They also do not provide shock absorption or heel cushioning which can be problematic for your feet. Additionally, you may suffer from glass cuts, puncture wounds, and stubbed toes since they offer little protection for your feet.
More Reasons Why They Are Bad for Your Feet
- They Slow You Down
- May Cause Blisters and Calluses
- Expose Your Feet to Bacteria
If you have any questions, please feel free to contact our offices located in The Woodlands and Woodville, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.