The Woodlands
Woodville(936) 273-3311
Items filtered by date: April 2019
How to Care for Wounds
 When existing wounds are treated promptly and correctly, there is a difference between a quick recovery and a longer healing time. It is helpful to wash the surface of the wound with salt water, followed by wiping the area with sterile gauze. If bleeding is present, it is helpful to apply pressure to the affected area. This is often accomplished by covering the wound with a dry cloth, and exerting pressure on it for several minutes. Research has indicated it is beneficial to cover moist wounds with dressings, and this may accelerate the healing process. If you have wounds on your feet, it is suggested to be under the care of a podiatrist, who can guide you toward proper wound care.
When existing wounds are treated promptly and correctly, there is a difference between a quick recovery and a longer healing time. It is helpful to wash the surface of the wound with salt water, followed by wiping the area with sterile gauze. If bleeding is present, it is helpful to apply pressure to the affected area. This is often accomplished by covering the wound with a dry cloth, and exerting pressure on it for several minutes. Research has indicated it is beneficial to cover moist wounds with dressings, and this may accelerate the healing process. If you have wounds on your feet, it is suggested to be under the care of a podiatrist, who can guide you toward proper wound care.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Dr. James Kutchback from James Kutchback, DPM, ABLES, CWS-P. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our offices located in The Woodlands and Woodville, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about Wound CareTypes of Foot Pain
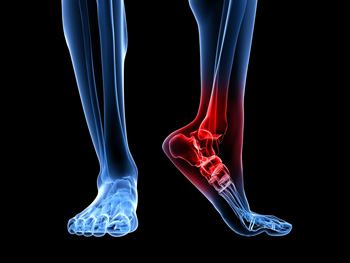 Many people experience heel pain at some point in their lives. Research has indicated that the most common form of heel pain is known as plantar fasciitis. This condition develops when the tendon that connects the heel to the toes becomes inflamed and irritated. Possible causes for this may be flat feet or if the arch is exceptionally high. Sever’s disease is a foot condition that may be experienced by teenagers who frequently participate in sporting activities. When this occurs, trauma is inflicted in the growth plate of the heel bone and may result in pain and discomfort. The Achilles tendon connects the heel bone to the calf muscles, and if this should become torn, pain is generally felt in the heel of the foot. If you are experiencing any type of foot pain, it is strongly suggested that you consult with a podiatrist who can properly diagnosis and treat your foot condition.
Many people experience heel pain at some point in their lives. Research has indicated that the most common form of heel pain is known as plantar fasciitis. This condition develops when the tendon that connects the heel to the toes becomes inflamed and irritated. Possible causes for this may be flat feet or if the arch is exceptionally high. Sever’s disease is a foot condition that may be experienced by teenagers who frequently participate in sporting activities. When this occurs, trauma is inflicted in the growth plate of the heel bone and may result in pain and discomfort. The Achilles tendon connects the heel bone to the calf muscles, and if this should become torn, pain is generally felt in the heel of the foot. If you are experiencing any type of foot pain, it is strongly suggested that you consult with a podiatrist who can properly diagnosis and treat your foot condition.
Many people suffer from bouts of heel pain. For more information, contact Dr. James Kutchback of James Kutchback, DPM, ABLES, CWS-P. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our offices located in The Woodlands and Woodville, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Symptoms of Morton’s Neuroma
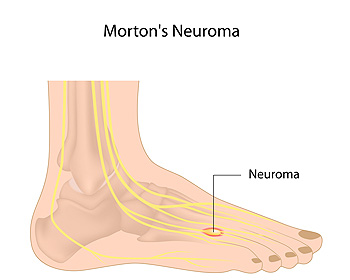 The place on the foot where pain from Morton’s neuroma is typically felt is the bottom of the third and fourth toes. This condition can develop as a result of a swollen nerve in the ball of the foot. Some of the symptoms that patients may experience can include numbness or a tingling sensation, a burning pain, or a feeling that something is inside the bottom of the foot. There are, however, some methods that can be implemented which may help in finding mild relief. These may include performing exercises to aid in strengthening and stretching the foot, in addition to massage therapy. Patients may also find comfort in resting the foot, or wearing shoes that have adequate room for the toes to move freely. If you have any kind of pain in your foot, it is suggested that you speak to a podiatrist who can properly diagnose and treat the cause.
The place on the foot where pain from Morton’s neuroma is typically felt is the bottom of the third and fourth toes. This condition can develop as a result of a swollen nerve in the ball of the foot. Some of the symptoms that patients may experience can include numbness or a tingling sensation, a burning pain, or a feeling that something is inside the bottom of the foot. There are, however, some methods that can be implemented which may help in finding mild relief. These may include performing exercises to aid in strengthening and stretching the foot, in addition to massage therapy. Patients may also find comfort in resting the foot, or wearing shoes that have adequate room for the toes to move freely. If you have any kind of pain in your foot, it is suggested that you speak to a podiatrist who can properly diagnose and treat the cause.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact Dr. James Kutchback of James Kutchback, DPM, ABLES, CWS-P. Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our offices located in The Woodlands and Woodville, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Ways to Alleviate Symptoms of Plantar Fasciitis
 Plantar Fasciitis refers to inflammation on the plantar fascia ligament, this ligament connects the heel to the toes. Overuse and strain can cause this condition, which affects the under arch of the foot and causes pain. This inflammation can also cause tension in surrounding muscles, and this can lead to the pain expanding into the calf. Stretches are beneficial in reducing tension, and therefore help to reduce overall pain. Towel curls can be performed by curling a towel with your toes. This stretch is done by placing a towel on the floor then while sitting, place your feet flat on the towel. By grasping the towel with your toes and curling inward you are stretching out the right parts of your foot. Foot flexes are also effective and are performed by sitting on the floor with your legs straight, then after wrapping an elastic band around your feet, begin to point your toes away from your body. If you believe you have plantar fasciitis, then it is highly recommended you speak to a podiatrist to learn about treatment options.
Plantar Fasciitis refers to inflammation on the plantar fascia ligament, this ligament connects the heel to the toes. Overuse and strain can cause this condition, which affects the under arch of the foot and causes pain. This inflammation can also cause tension in surrounding muscles, and this can lead to the pain expanding into the calf. Stretches are beneficial in reducing tension, and therefore help to reduce overall pain. Towel curls can be performed by curling a towel with your toes. This stretch is done by placing a towel on the floor then while sitting, place your feet flat on the towel. By grasping the towel with your toes and curling inward you are stretching out the right parts of your foot. Foot flexes are also effective and are performed by sitting on the floor with your legs straight, then after wrapping an elastic band around your feet, begin to point your toes away from your body. If you believe you have plantar fasciitis, then it is highly recommended you speak to a podiatrist to learn about treatment options.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. James Kutchback from James Kutchback, DPM, ABLES, CWS-P. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact our offices located in The Woodlands and Woodville, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about Plantar Fasciitis
How to Prevent Athlete’s Foot
 The symptoms of a condition that is referred to as athlete’s foot may consist of dry, flaky and cracked skin between the toes or on the soles of the feet. It is typically caused by a fungus which thrives in warm and moist areas. These may include public swimming pools, shower room floors, or locker rooms. It is known to be extremely contagious, and there are measures that can be implemented to avoid contracting athlete’s foot. These may consist of wearing appropriate shoes in public areas, and keeping your shoes and socks dry. Additionally, it may be helpful to wash and dry your feet daily, followed by utilizing a powder between the toes. This may aid in keeping the feet dry. If you have athlete’s foot, it is advised to consult with a podiatrist who can properly diagnosis and treat this condition.
The symptoms of a condition that is referred to as athlete’s foot may consist of dry, flaky and cracked skin between the toes or on the soles of the feet. It is typically caused by a fungus which thrives in warm and moist areas. These may include public swimming pools, shower room floors, or locker rooms. It is known to be extremely contagious, and there are measures that can be implemented to avoid contracting athlete’s foot. These may consist of wearing appropriate shoes in public areas, and keeping your shoes and socks dry. Additionally, it may be helpful to wash and dry your feet daily, followed by utilizing a powder between the toes. This may aid in keeping the feet dry. If you have athlete’s foot, it is advised to consult with a podiatrist who can properly diagnosis and treat this condition.
Athlete’s Foot
Athlete’s foot is often an uncomfortable condition to experience. Thankfully, podiatrists specialize in treating athlete’s foot and offer the best treatment options. If you have any questions about athlete’s foot, consult with Dr. James Kutchback from James Kutchback, DPM, ABLES, CWS-P. Our doctor will assess your condition and provide you with quality treatment.
What Is Athlete’s Foot?
Tinea pedis, more commonly known as athlete’s foot, is a non-serious and common fungal infection of the foot. Athlete’s foot is contagious and can be contracted by touching someone who has it or infected surfaces. The most common places contaminated by it are public showers, locker rooms, and swimming pools. Once contracted, it grows on feet that are left inside moist, dark, and warm shoes and socks.
Prevention
The most effective ways to prevent athlete’s foot include:
- Thoroughly washing and drying feet
- Avoid going barefoot in locker rooms and public showers
- Using shower shoes in public showers
- Wearing socks that allow the feet to breathe
- Changing socks and shoes frequently if you sweat a lot
Symptoms
Athlete’s foot initially occurs as a rash between the toes. However, if left undiagnosed, it can spread to the sides and bottom of the feet, toenails, and if touched by hand, the hands themselves. Symptoms include:
- Redness
- Burning
- Itching
- Scaly and peeling skin
Diagnosis and Treatment
Diagnosis is quick and easy. Skin samples will be taken and either viewed under a microscope or sent to a lab for testing. Sometimes, a podiatrist can diagnose it based on simply looking at it. Once confirmed, treatment options include oral and topical antifungal medications.
If you have any questions, please feel free to contact our offices located in The Woodlands and Woodville, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.

